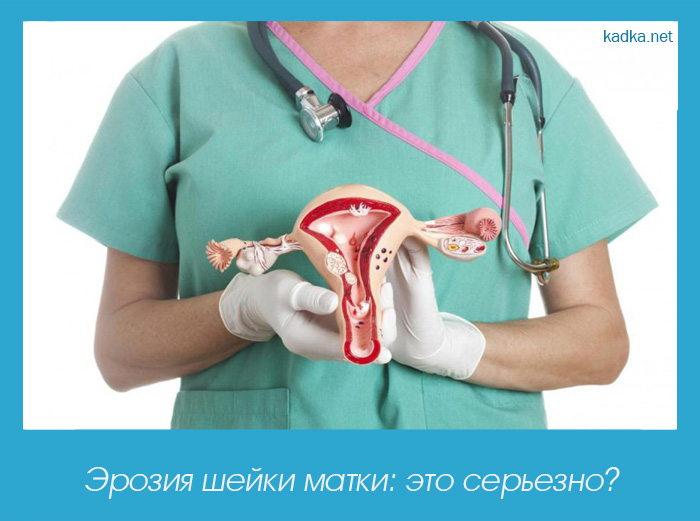
Lower Back Pain: Causes and Treatment
In most cases, lower back pain is caused by exposure to cold or muscle strain resulting from awkward movements or heavy lifting, and may resolve on its own. However, if the pain interferes with your daily life, does not improve for a long time, or is accompanied by other concerning symptoms, you should consult a doctor for diagnosis and treatment of lower back pain.
Article Contents:
Depending on how long the pain has been bothering the patient, doctors distinguish between:
This note is for informational purposes only. Treatment is prescribed by a specialist after consultation. Acute pain — less than 4 weeks Subacute pain — 4 to 12 weeks Chronic pain — more than 12 weeks
When using this method, the doctor notes that the patient simply has back pain: this may be a stabbing pain during movement, intermittent back pain, constant dull pain, sharp stabbing pain, and other irritating sensations of varying intensity. Depending on the duration, location, and nature of the pain, the doctor suggests what is actually considered the cause.
Lower Back Pain: Causes
Pain in the lower back may be related to issues with the spine, for example, or to other organs and systems in the body. To understand how to treat lower back pain, it is necessary to determine the exact cause of the pain.
Vertebrogenic pain, caused by spinal disorders, includes:
Osteochondrosis, manifested by problems with the intervertebral discs, facet joints, or facet joints. These changes occur in everyone as they age: intervertebral discs lose water and elasticity, while facet joints become denser and less mobile
Overuse of the muscles and ligaments of the spine Compression of the spinal nerve roots—radiculopathy Spinal trauma Spinal instability due to weakness of the musculoskeletal system Non-vertebrogenic conditions include: Neurological disorders:
- Lumbosacral plexopathies are damage to the nerve plexus from which the peripheral nerves of the lower extremities originate. They occur in cases of trauma, metabolic disorders, and medication use;
- Dystonia — a disorder of the muscle tone supporting the spine. In this case lower back pain may be accompanied by poor posture. The condition may be congenital.

Systemic diseases:
- Infections affecting the vertebrae, intervertebral discs, the spinal cord membranes, or the spinal cord itself, such as osteomyelitis or epidural abscess;
- Malignant and benign tumors, metastases;
- Osteoporosis—a decrease in the density of skeletal bone tissue, which can lead to vertebral fractures;
- Rheumatic diseases, such as inflammatory spondyloarthropathy or ankylosing spondylitis.
Pain originating from internal organs. It is caused by factors outside the spine and radiates to the lower back, sometimes to the center, sometimes to the side, depending on the affected organ. These include:
- Gastrointestinal disorders—most commonly pancreatitis;
- Diseases of the urinary system—infections such as pyelonephritis and urolithiasis. Severe paroxysmal shooting pains in the back and side accompany renal colic when a stone moves through the ureter;
- Aortic aneurysm — a rare, dangerous condition in which the wall of the body’s largest artery bulges. This can cause a pulsating sensation in the abdomen;
- Hip joint disorders—injuries, inflammation, degeneration.
Psychogenic pain: Lower back pain may be accompanied by anxiety or depression.
- Herniated disc;
- Trauma;
- Malignant or benign tumor;
- Infection.

Symptoms
Lower back pain is often nonspecific, meaning it is caused by a benign condition of the musculoskeletal system. In such cases, patients report the following symptoms:
Aching, pulling, or pressing pain
The onset or worsening of pain when a person stands or sits for a long time, lifts something heavy, performs physical work with raised arms (e.g., hanging curtains, changing light bulbs in a chandelier), or bends over repeatedly and for long periods (e.g., when mopping the floor, vacuuming, or shoveling snow)
Absence of other symptoms
Red flags indicate that the pain may be a symptom of a dangerous condition:
Age over 50. This age group has a higher risk of developing osteoporosis and tumors.
Pain at rest and at night, disrupting sleep. Nonspecific pain usually occurs with movement or prolonged static strain but disappears after resting in a comfortable position
General weakness—also not typical of nonspecific pain
Unexplained weight loss in recent months. May be a sign of persistent systemic inflammation in the body caused by autoimmune diseases or tumors
Elevated body temperature, chills. Indicates severe inflammation of various causes. Severe or progressive loss of sensation or weakness in the leg muscles
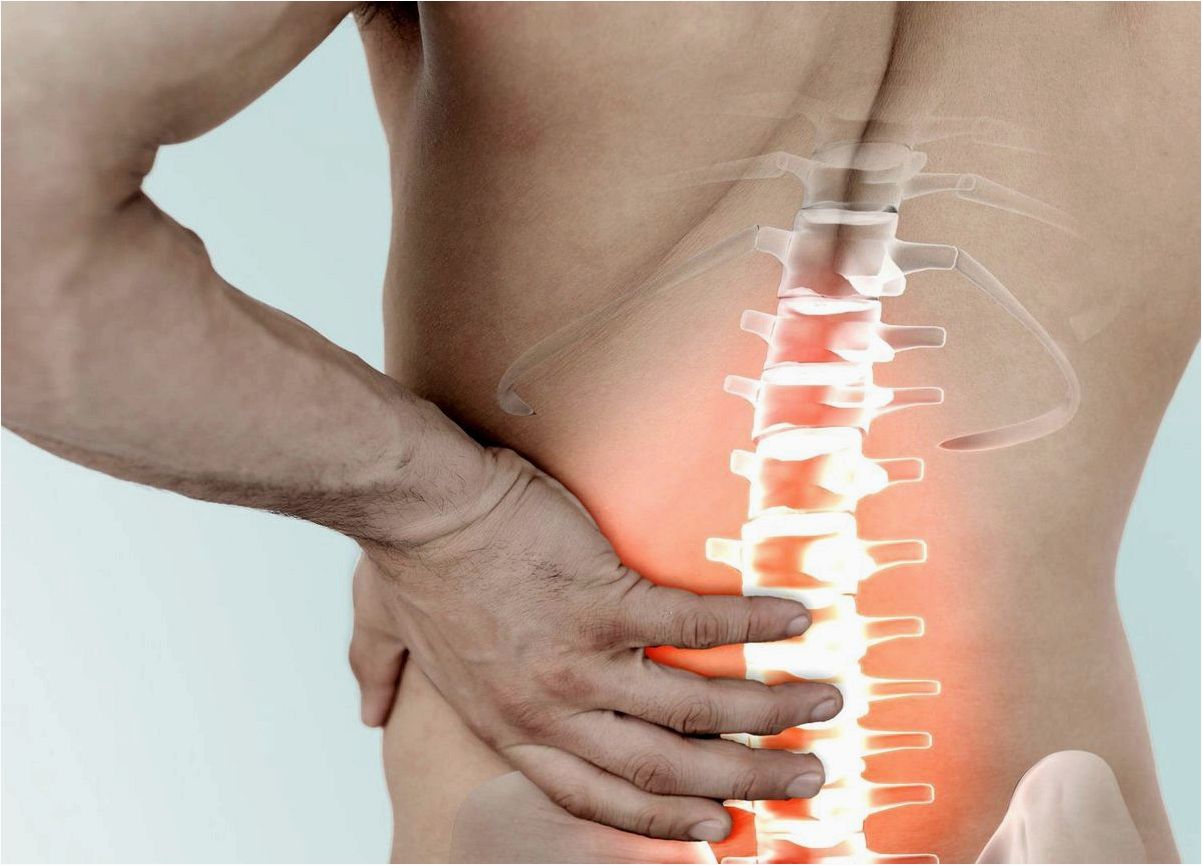
Abnormal bladder or bowel function—this includes involuntary urination or, conversely, difficulty urinating or constipation. Nerves from the lower spinal cord extend to the pelvic organs and lower limbs. For example, they contain both motor and sensory fibers. Loss of sensation or movement combined with acute pain is a symptom of nerve compression and, possibly, spinal cord compression. If you do not seek medical attention with such symptoms, the function of the nerve or the affected area of the spinal cord may be lost permanently.
Lack of improvement following recovery and the transition of acute pain to chronic pain
Specifics of the medical condition. For example, if lower back pain is observed in a patient with a previously diagnosed case of osteoporosis or a malignant tumor. In this case, it does not matter how long ago the diagnosis was made. Or if the pain was noticed in a person who recently suffered a serious infection, surgery, or a weakened immune system, which, for whatever reason, resolved quickly. In these cases, lower back pain may indicate various complications.
If you identify even one of the listed symptoms in yourself, consult a doctor immediately for further examination.
Diagnosis
- Laboratory tests — Complete blood count, blood chemistry panel, urinalysis, tests for infections and autoimmune diseases;
- Electroneuromyography — A study of impulse conduction along nerve fibers, which allows for a visual representation of the affected area in cases of neurological disorders;
- Imaging using X-rays, computed tomography (CT), and magnetic resonance imaging (MRI), which will undoubtedly be helpful;
- Ultrasound examination of the kidneys and abdominal cavity — these are performed when internal organ pathology is suspected;
- Bone assessment: densitometry—when osteoporosis is suspected; bone scintigraphy—in cases of malignant lesions.
Often, when experiencing lower back pain, people do not see a doctor and instead go on their own to get an MRI of the spine. This situation can confuse the patient: studies have indeed shown that most middle-aged people have asymptomatic spinal hernias. The patient attributes the pain to the MRI and does not seek further medical care. As a result, the person endures discomfort for a long time and takes painkillers indiscriminately, leading to stress and side effects.
Which Doctor to See
Initially, for mild back pain, you can see a general practitioner. They will determine the cause of the pain and, depending on that, refer you to another specialist. You can skip this step and make an appointment with a neurologist right away.
Neurologists and orthopedists at the clinic diagnose and treat lower back pain, neurological disorders, and hip joint problems. There is also a more specialized field—vertebrologist, who specializes in spinal disorders.
- Rheumatologist;
- Surgeon;
- Urologist;
- Gastroenterologist;
- Endocrinologist;
- Oncologist.
If a mechanical injury is diagnosed, specialists in therapeutic exercise, reflexology, physical therapy, and massage therapy will undoubtedly assist in the patient’s treatment.
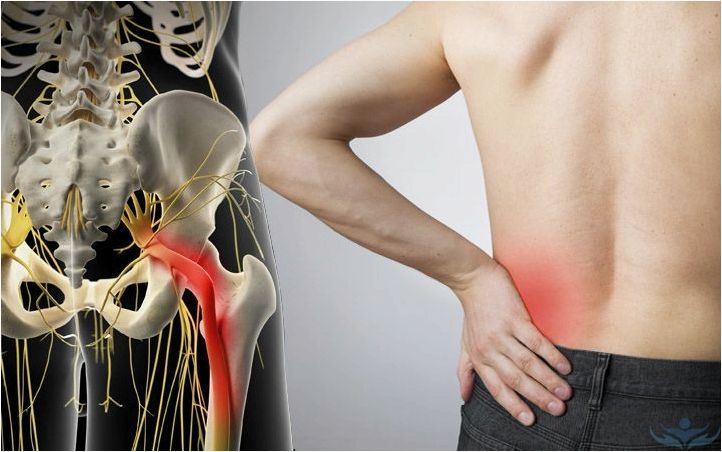
Schedule a consultation with a neurologist
The session lasts 60 minutes and combines diagnosis, review of your MRI, and the development of a treatment plan; therefore, it is conducted in real time, for example, online.
How to Treat Lower Back Pain
Surgical treatment is primarily used in cases of spinal cord or spinal nerve compression, particularly if the patient experiences limb weakness or urinary dysfunction. These symptoms are likely caused by a herniated disc, a tumor, or trauma. A consultation with a neurosurgeon may be recommended for patients with acquired pain when conservative treatment over 12 months has been ineffective. The decision to operate is made only after spinal imaging.
In fact, studies have shown that uncomplicated disc herniations can be successfully treated without surgery, using conservative methods. Rehabilitation programs achieve good results in 90% of patients with chronic back pain.
Conservative treatment combines both pharmacological and non-pharmacological methods.
Medication-based treatment involves the use of nonsteroidal anti-inflammatory drugs (NSAIDs), which relieve pain and inflammation and help relax the muscles.
- Physical therapy aims to quickly alleviate pain and inflammation, as well as to promote tissue healing and muscle relaxation. More effective methods include: magnetic therapy, laser therapy, and shockwave therapy;
- Acupuncture—the insertion of special sterile needles into specific points to reduce pain and relax muscles;
- Massage — improves mobility of the spine and joints, and helps distribute the load on the back muscles correctly;
- Physical therapy — helps relax and restore the back muscles. Exercises are effective for both acute and chronic back pain.
If a patient’s pain persists for more than 12 months, it is classified as chronic. During treatment, antidepressants with analgesic effects and cognitive-behavioral therapy are added to all of the above methods.
Bed rest has not been shown to be superior in the treatment of mechanical low back pain and is not considered a viable alternative to the methods listed above. Rather, it follows the path of neglect, which is highly likely for the patient. Prolonged bed rest leads to joint stiffness, muscle tension, and, most importantly, slows down recovery.