Laser Vision Correction Methods
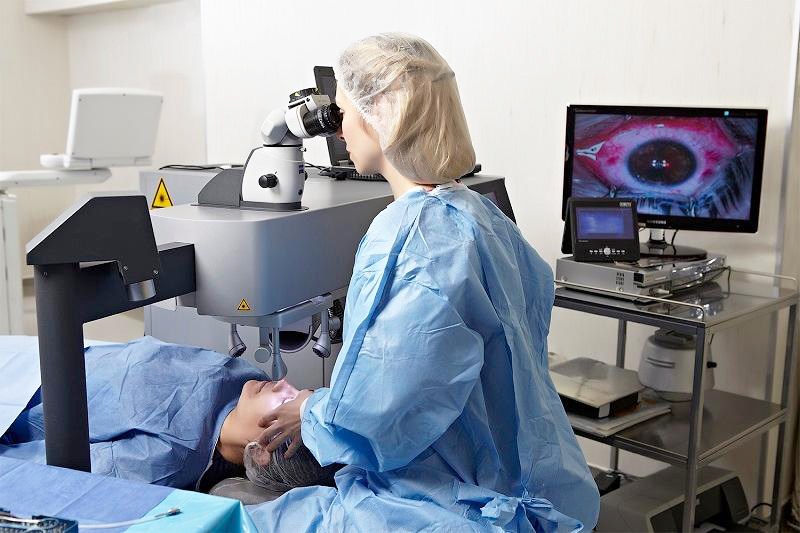
Astigmatism, myopia, and hyperopia are refractive errors of the visual system that affect a large number of people. Laser vision correction offers patients with these eye conditions the opportunity to permanently stop wearing contact lenses or glasses. At the “Zrenie 2100” clinic https://korrektsiya-zreniya.ru/moskva/ experienced doctors have already performed at least 1,000 eye surgeries. Although most of the procedure is performed automatically by the laser, the doctors have extensive experience with laser surgery, allowing them to successfully treat even the most complex cases.
Surgical intervention using laser technology makes it possible to target only the shape of the cornea and correct its irregularities. After the procedure, visual acuity is restored, allowing patients to see clearly again.
Laser refractive surgery is constantly evolving, with new equipment and surgical techniques emerging, and the positive results demonstrate the safety and long-lasting effects of the procedure.
The speed of the procedure and the fact that hospitalization is not required are also considered among the main advantages of this type of correction—all treatment is performed on an outpatient basis. Preoperative preparation, the surgery itself, and the initial assessment of results take about 2 to 3 hours; patients then leave the clinic on their own and return to their normal routine within a few days.
Indications for laser vision correction
The procedure for correcting refractive errors using laser technology is recommended for virtually all patients with similar conditions. Restrictions apply only to severe cases, although the latest-generation laser systems ensure maximum effectiveness.
LASIK laser vision correction is used to treat the following eye conditions:
- Hyperopia from +1 to +6 diopters—a condition affecting near vision.
- Myopia fro m-1 t o-15 diopters—difficulty seeing objects at a distance.
- Astigmatism from 1 to 4 diopters is a difference in the refraction of light rays across different meridians of a single eye.
- Mixed astigmatism is a combination of farsightedness and nearsightedness.
Other specific indications include intolerance to contact lenses due to allergies or other medical conditions, as well as difficulties in wearing glasses on a regular basis due to the nature of one’s professional activities. Laser vision correction can also be performed on patients with a condition affecting only one eye.
Preparation for Surgery
The determination of indications for the procedure and the likelihood of its success is carried out during a consultation with an ophthalmologist, who assesses the condition of the visual system. Only after a complete examination, the completion of all diagnostic tests, and the establishment of a final diagnosis can you evaluate the expected outcome and risks of laser vision correction.
After ruling out any contraindications to refractive surgery, a series of additional eye examinations are performed, and the patient undergoes a blood test.
Signing a consent form is mandatory—the patient must be fully informed about the laser vision correction procedure, all possible risks, and potential outcomes.
A patient who decides to undergo surgery must actively participate in the process and assist the surgeons as much as possible. They must strictly follow the doctor’s recommendations at all stages of preparation, during the procedure, and afterward.
It is important to remember that you should not wear contact lenses for two weeks prior to the procedure, as the cornea needs to return to its natural position, which is altered by the use of lenses.
You should also avoid alcohol for a few days beforehand—it causes dry eyes and may interfere with the effectiveness of the anesthetics.
On the day of the procedure:
- You must bring all medical documents and your passport;
- All cosmetics must be thoroughly removed. Young women should not wear makeup—the skin around the eyes and eyelids must be completely clean;
- The use of cologne is prohibited;
- you should bring sunglasses—you will need them after the procedure.
What is required of the patient during laser vision correction:
- relax the muscles of your entire body as much as possible;
- focus on the red spot and do not take your eyes off it;
- Do not worry about pain relief—the effect of the anesthetic drops will definitely last; for this reason, they are administered twice;
- do not forget that you must not compromise sterility or touch your face with your hands;
- avoid sudden movements—laser vision correction is performed under a microscope, and any shift in the patient’s body position interferes with the surgeon’s work;
- Be prepared for a red spot to appear in your field of vision for 10–15 seconds;
- Try to remain calm and maintain a positive attitude.
There are several main methods of laser vision correction. They differ in the type and model of laser used, as well as in the procedure itself.
How laser vision correction is performed
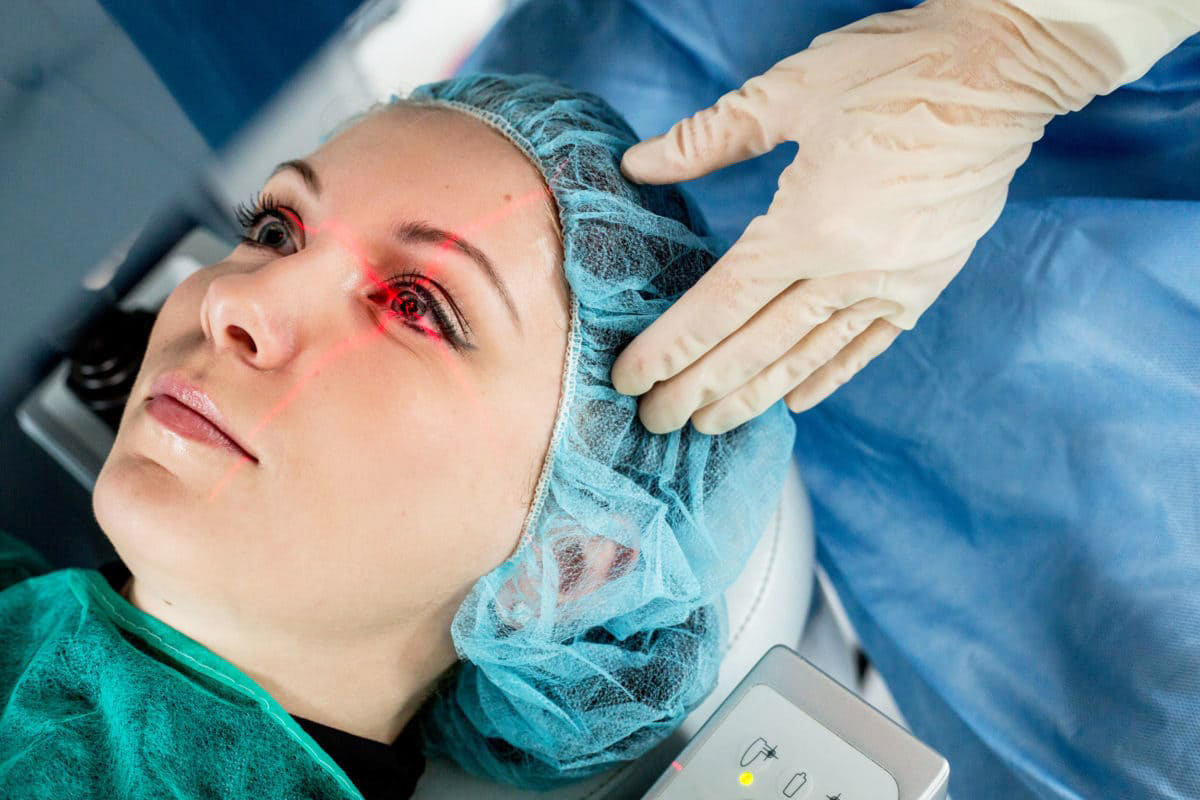
Accompanied by medical staff, the patient enters the operating room—a nurse instructs them on how to behave in order not to compromise the sterile environment. Once preoperative preparation is complete, the patient is asked to lie down comfortably on a special couch, with their head resting in a special recess and their arms positioned strictly along the body.
The laser vision correction process can be broadly divided into several stages:
- Preparation. The procedure is performed under local anesthesia—anesthetic eye drops are used for this purpose. The medication takes effect immediately after instillation. Next, a special device is applied to hold the eyelids open—an eyelid speculum. This device prevents the patient from blinking or closing their eyes, which is crucial during the procedure. The patient must focus on a red dot directly in front of them at all times.
- The corneal flap creation stage. In order to work on the deeper structures of the cornea, access to them must be ensured. A microkeratome or femtosecond laser creates a corneal flap with a diameter of about 9–10 mm—this flap is moved aside for the duration of the procedure. It is at this moment that the red flashing spot disappears—the patient is always warned about this so they do not become frightened.
- The procedure. The direct application of the laser to the structures of the cornea is the most critical stage. Performing these procedures requires the ophthalmic surgeon to possess special skills, experience, and maximum concentration on the treatment process. The patient simply needs to lie still and focus their gaze on the flashing red spot; nothing else is required. The laser acts on the cornea according to a specific protocol—this procedure has been thoroughly tested and refined, so there is no need to worry about the accuracy of the procedure. The laser beam is applied for approximately 1–5 seconds, during which the patient hears the characteristic sounds of the device operating.
- Conclusion. After the shape of the cornea has been altered, the flap of its outer layer is repositioned, and a special solution is instilled into your eyes. No stitches are required—the unique structure of the cornea allows for the protective layer to heal on its own. After a few minutes of rest, the eyelid speculum is removed, signaling the end of the procedure. It is very important not to rush to close your eyelids tightly or move your eyes—immediately after the procedure, any pressure on the eyeball is contraindicated.
- The initial postoperative period. For the first few hours after surgery, the patient remains under close medical supervision—this allows for an assessment of the initial results of the laser correction and ensures the procedure’s safety. After a couple of hours, you may go home, preferably accompanied by a loved one. On a sunny day, wear protective eyewear. During the initial recovery period, it is important to follow the ophthalmologist’s recommendations and schedule a follow-up appointment.
Postoperative period
The immediate postoperative period begins right after surgery—the patient remains under medical supervision for the first couple of hours. Although visual acuity returns almost immediately, there may be some discomfort—such as seeing “floaters” in front of the eyes, blurred vision, a foreign body sensation, eyelid swelling, light sensitivity, burning, or tearing. These symptoms may persist for several hours or, in some cases, up to a day after surgery.
For this reason, it is important for the patient to have a companion with them—they can help ensure a safe trip home from the hospital and assist in following the doctor’s instructions. You should remember the sequence of medication use and follow all of the ophthalmologist’s recommendations.
You can divide the subsequent rehabilitation period into the following stages:
- The early period lasts for the first few days after surgery—you must visit the clinic to monitor the condition of the eye and restore visual function. During this period, restrictions are the strictest—any physical activity, washing your face, alcohol consumption, working at a computer, and driving are prohibited.
- In two weeks, the restrictions will be eased, and you will be allowed to wash your hair carefully, provided you follow safety precautions and take care to prevent chemical compounds and cosmetics from getting into your eyes. You can gradually return to your normal work schedule, but you should avoid work that involves excessive visual strain. However, you should still avoid alcohol and cosmetics. It is also prohibited to be in the sun without sunglasses or to visit swimming pools and saunas.
- After one month, the shape of the cornea is fully stabilized, and all restrictions and prohibitions are lifted. The patient can now enjoy normal activities, seeing objects clearly and sharply without contact lenses or glasses.
Possible Complications
No field of medicine can guarantee the absence of complications. Since the success of any medical procedure depends on many internal and external factors, it is impossible to predict the results with absolute certainty. However, statistics show that only 0.01% of patients experience complications from laser vision correction.
The most common adverse effects of the procedure:
- swelling;
- bleeding;
- keratitis and other inflammations of the eye structures;
- various injuries to the eye;
- ingrowth of epithelial structures under the corneal flap;
- overcorrection or undercorrection of refractive error;
- temporary impairment of night vision;
- displacement of the excised corneal flap.
Any complications are generally reversible and can be treated under the close supervision of a specialist. The doctor is required to warn patients about potential risks during the preoperative consultation and does everything possible to prevent complications from developing. Laser vision correction is rightly considered minimally invasive and as safe as possible. In addition, thorough preparation for the procedure and strict adherence to all of the ophthalmologist’s postoperative recommendations help prevent adverse outcomes.