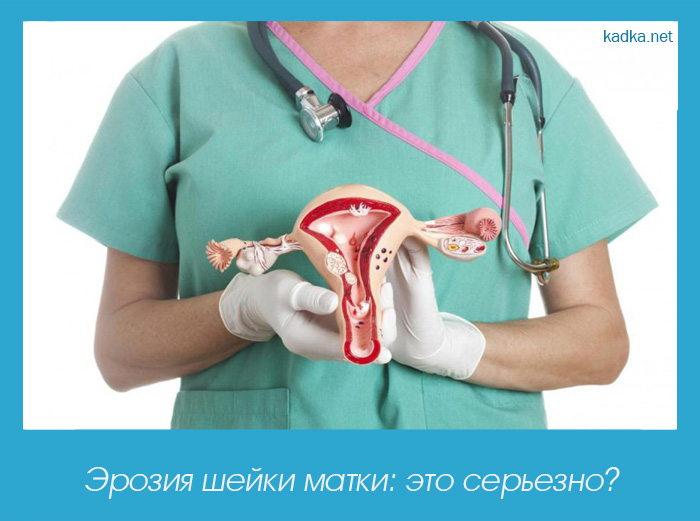
Removal of Cervical Polyps
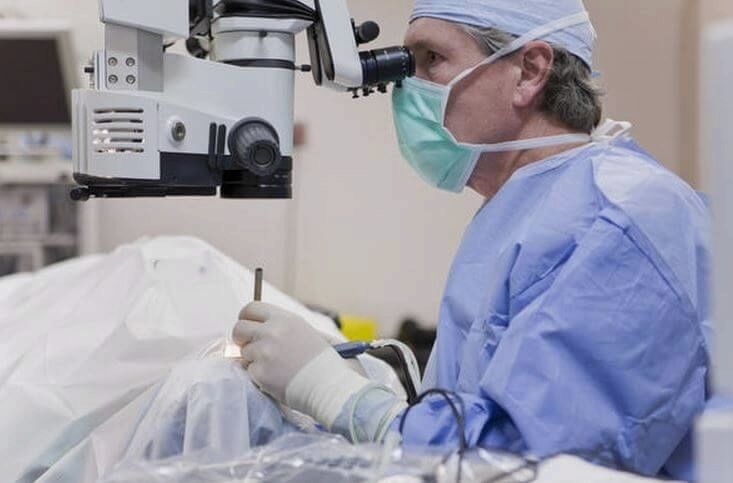
A cervical polypectomy is a surgical procedure that involves removing a growth from the upper layer of the uterine lining. The purpose of the procedure is to address thickening of the lining or to identify polyps on its surface. Before scheduling a polypectomy, a comprehensive evaluation of the patient’s health is conducted, and the woman’s individual physiological characteristics are taken into account during the procedure.
Why is this procedure necessary?
Polyps are the result of abnormal growth of endometrial tissue, which affects a woman’s well-being and the normal processes occurring in her body. Polyps develop against a background of severe inflammatory processes, when a woman suffers from urogenital infections or does not maintain proper personal hygiene.
In most cases, polyps appear in the upper layers of the mucous membrane and grow rapidly. The formation of polyps is accompanied by severe pain. Polypectomy not only eliminates the underlying cause of the health problem but also relieves associated symptoms. Both adult women and girls are at risk of developing polyps.
Contents:
- Why is this procedure necessary?
- Indications for the procedure
- Preparation process
- Additional diagnostics
- Why is polypectomy performed on an urgent basis?
- Removal of Cervical Polyps
- Polypectomy of Fibrous Lesions
- Possible Complications
- Recovery After the Procedure
- Home Care
Indications for the procedure
The primary indication for surgical intervention is the formation and growth of polyps. This condition negatively affects the patient’s well-being, menstrual cycle, and quality of intimate life. As the disease progresses, it calls into question the patient’s ability to conceive and carry healthy children to term. Since polyps have stalks that penetrate the inner layers of the mucous membrane, polypectomy is the only viable option for removing the growths.
Over time, without proper treatment, the stalks grow toward the blood supply and feed on blood, allowing the polyps to continuously nourish themselves and grow. The number and size of polyps directly depend on the woman’s physical condition. The formation of polyps is common among women following an abortion. If a woman has not undergone proper post-abortion recovery, she is prescribed a polypectomy. The primary cause of growths on the uterine lining is hormonal imbalance.
Patients with severe inflammation and established polyps should undergo a polypectomy. Due to the prolonged inflammatory process, it is necessary to treat it with radical methods. Patients with postpartum trauma also require surgical intervention. Regardless of the cause of the polyp, a polypectomy is performed to improve the woman’s condition, followed by appropriate rehabilitation and preventive care.
Preparation process
For polyp removal several procedures are used, including curettage and cauterization. The drawbacks of such methods can affect the patient’s well-being and her subsequent recovery. To prepare the woman’s body, a thorough diagnostic evaluation must be conducted to establish an accurate diagnosis and identify any underlying conditions or chronic pathologies.
Before performing a polypectomy, an obstetrician-gynecologist examines the uterus. In addition, an ultrasound examination (sonography) and colposcopy are ordered. These diagnostic methods allow for an assessment of the patient’s overall health. Identifying any contraindications to surgical intervention is the primary responsibility of the attending physician. During hysteroscopy, an accurate diagnosis can be made and the need for polypectomy confirmed. Metrography (ultrasound imaging of the uterus) allows for an assessment of the condition of the mucous membrane and the extent of its damage.
Prior to polypectomy, a diagnostic uterine curettage is performed, and the obtained material is sent for further histological examination. Only a comprehensive approach to solving the problem ensures a stable and positive outcome. No polypectomy is performed without preparation and subsequent rehabilitation.
Additional diagnostics
A comprehensive diagnostic examination is performed immediately before polypectomy. During the examination, the attending physician decides on the further course of the procedure. The patient is prescribed:
- blood tests;
- urinalysis;
- smears;
- ultrasound;
- contrast-enhanced ultrasound.
Polyps removed during a polypectomy may present symptoms similar to those of other conditions. Signs of a growing growth can be mistaken for uterine fibroids or adenomyosis. Only a treating physician can make an accurate diagnosis and prescribe a procedure to remove the abnormal growth. Patients should not schedule a polypectomy on their own.
Why is polypectomy performed on an urgent basis?
Polyps are dangerous growths on the surface of the uterus that can harm women of any age. Cystic polyps are benign growths that can grow and increase in size without proper treatment. In the early stages, these growths are not dangerous, but the larger the polyp, the higher the risk of developing cancer.
Atypical polyps are a precancerous condition that requires urgent treatment. The longer a woman delays having the polyps removed, the more difficult it will be for her to recover after surgery. Without comprehensive treatment, their formation against a background of hormonal imbalances can lead to infertility in patients. Polypectomy is an essential procedure to halt the disease. The main growths are removed through surgical intervention. Polypectomy is recommended for pregnant women with polyps growing in the uterus. Your doctor will assess the risk to both mother and child.
Removal of Cervical Polyps
Several methods are used simultaneously to treat polyps. Polypectomy is performed in combination. Otherwise, it is impossible to achieve good results. Immediately after thorough preparation, the patient undergoes the procedure: during the operation, the cervix is grasped with bullet forceps. The method of grasping the polyp depends on the structure of the polyp’s stalk.
If the stalk is thin (protruding or visible in the cervical canal), it must be removed using a twisting motion. The procedure differs for smaller growths. All polyps are rotated in the same direction around their axis. In such cases, forceps are used to grasp the stalks. If the polyps protrude from the mucosa, a 5% iodine tincture is applied to the mucosa. If multiple polyps are present and there are no contraindications, additional probing is performed, followed by curettage of the endometrium.
Polypectomy of Fibrous Lesions
Fibrous polyps are characterized by a thin stalk that is difficult to remove. Torsion techniques are used to grasp it during polypectomy. If the polyp is large and covers a significant area of the damaged mucosa, large forceps are used to remove the layers. In such cases, an anterior hysterectomy is performed. If thick stalks are present in the fibrous growth during polypectomy, they are removed without additional twisting. Due to the thicker spinal roots, the uterus may be inverted, which is something that is generally avoided during the procedure.
After removing part of the polyp, the tumor capsule is incised with scissors. Only after this step is the remaining portion of the tissue removed. A simple incision at the base of the vertebra does not yield results as good as those of a complex polypectomy. This procedure reduces the likelihood of intrauterine bleeding. Dissection of the tumor reduces the risk of vascular damage.
Possible Complications
The consequences of polypectomy pose a risk to the woman and her body. During the operation, bleeding may occur from the site of the excised tumor. If bleeding begins during the operation or blood vessels are damaged, the damaged tissues must be ligated. For this purpose, the bleeding area of the uterus is ligated with a piece of cut intestine. In some cases, the bleeding vessels must be ligated for 10–12 hours. The same measures are used to stop bleeding in the stretched cervix.
Uterine inversion is the result of an improperly performed surgery. If the thick stalk of the polyp is not completely removed or pulled out correctly during polypectomy, the uterus will invert. Special care must be taken during the procedure, especially if the polypectomy is performed during pregnancy.
Uterine damage is a serious complication of polypectomy. Improper removal of polyps with thick stalks can cause damage. If an incision is not made before removing the polyp capsule, this can lead to damage to the uterine wall. An improperly removed stalk can cause hemorrhage. Polypectomy is a complex procedure requiring highly skilled surgeons and medical staff.
Recovery After the Procedure
After polypectomy, patients need rest and relaxation. Postoperative pain can last up to two to three weeks, and in some cases, up to a month. Heavy bleeding indicates dangerous complications from the procedure: uterine spasms accompanied by light bleeding.
During the postoperative period, patients are prescribed pain medications. To help with recovery, women who have undergone a polypectomy are prescribed a course of anti-inflammatory drugs and antibiotics. Antimicrobial drugs are part of preventive measures. Two weeks after the polypectomy, a follow-up ultrasound is performed to monitor the healing of the mucous membrane.
Home Care
After a polypectomy, patients recover at home over an extended period of time. For the first few weeks, women should not use douches or tampons. Hot baths and saunas are prohibited. Such activities can lead to uterine bleeding. During the recovery period, strenuous physical activity and visits to the gym should be avoided. Sexual intercourse is not recommended until full recovery. The recovery time after polypectomy and additional procedures varies from person to person.